Surgery is used to treat many colon and rectum problems and diseases. Depending on the case, a surgeon may use traditional (open) or minimally invasive procedures. The field of minimally invasive colon and rectal surgery is currently evolving. Every year brings new information based on further refinements and increasing use of these techniques.
Minimally Invasive Colon and Rectal Surgery
Traditional open surgeries typically involve doctors making an incision 6 to 12 inches long, large enough to offer good sight, access to the abdominal organs, and the use of hand-held surgical equipment.
Minimally invasive surgery is designed to perform operations through smaller incisions, which minimizes the discomfort and healing difficulties associated with long incisions. A range of common benign and malignant colon and rectal disorders can be efficiently treated with minimally invasive surgery. All minimally invasive surgical procedures need advanced surgical expertise along with specialized equipment. Surgeons are trained in performing minimally invasive surgery and can discuss the specific surgical procedures they recommend. All minimally invasive surgeries are conducted when the patient is treated with general anesthesia.
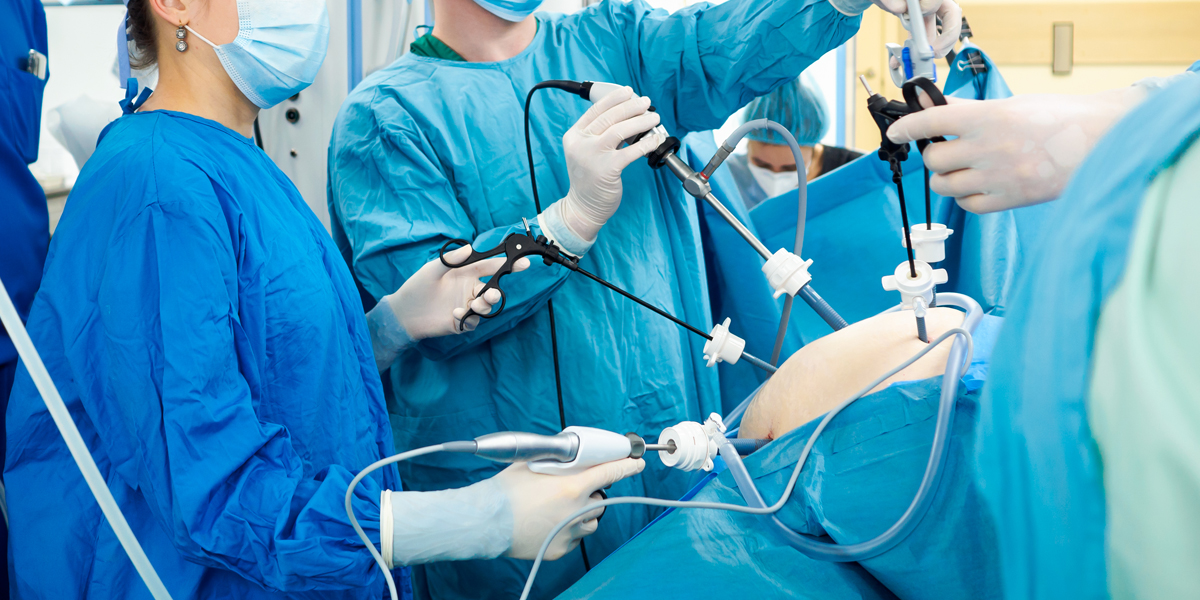
Laparoscopic surgery: The surgeon makes several small incisions, each approximately half an inch in size. A camera is put into one of the incisions during laparoscopic surgeries, allowing the surgeon to examine the inside of the belly on operating room monitors. The majority of colon and rectal surgeries require 2-4 additional incisions. To offer the surgeon more area to operate on, carbon dioxide gas is inflated to expand the abdomen for the procedure. Special equipment is inserted into the other small incisions to allow the surgeon to operate within the belly while viewing the cameras. To remove a section of the intestine from the abdomen for many colon and rectal surgeries, a slightly bigger incision (approximately 2-4 inches in length) is made to proceed.
Hand-assisted laparoscopic surgery: During this treatment, a device is inserted through a 3- to 4-inch incision. The surgeon inserts a hand into the incision to assist with the surgery during these laparoscopic procedures.
Single incision surgery or single-site surgery: The laparoscope and surgical equipment are both passed through a single, small incision in this procedure. This surgery is more commonly used than other laparoscopic surgeries.
All of the procedures described are known as “minimally invasive surgery,” but their overall benefits and complications differ slightly.
Benefits of minimally invasive surgery
The incisions are much smaller than in traditional surgery. Possible benefits include:
- less postoperative discomfort
- shorter stay at the hospital
- Pain relief after surgery
- Faster recovery
- Fewer surgical scars
It is important to note that long-term outcomes are similar between open and minimally invasive procedures. However, minimally invasive surgery provides advantages in the early post-surgical rehabilitation process.
Risks of minimally invasive surgery
Minimally invasive surgery has been extensively researched. Complications are as likely as in traditional open surgery. Every surgical treatment, whether minimally invasive or traditional, is concerned with the possibility of complications. Bleeding, infection, post-operative bowel blockage, and leaking from an intestinal anastomosis are all risks associated with both open and minimally invasive colon and rectal surgery. Other risks, such as heart problems, pneumonia, and blood clots, exist with any major abdominal surgery requiring general anesthesia.
Occasionally, a surgeon will find problems during surgery that make minimally invasive surgery too risky to continue. The incision is opened in this case to allow traditional surgical procedures to be used to complete the surgery. This is known as a “conversion” from traditional or “open” surgery, and it is considered a surgical decision rather than a complication.
It is necessary to consult with your surgeon about your medical condition and surgery options. You and your doctor can evaluate the risks and advantages of minimally invasive surgery compared with regular surgery. Minimally invasive surgery is not appropriate for all patients or conditions.
When is minimally invasive surgery an option?
Most abdominal, colon, and rectal operations may be done in a less invasive manner. Numerous studies have shown that minimally invasive surgery is a viable treatment option for colon cancer when performed appropriately. In general, minimally invasive surgery is suitable for rectal abnormalities in the hands of well-trained surgeons following accepted cancer surgery procedures.
The following factors help determine if a minimally invasive procedure can be performed safely and effectively.
- Prior surgical history.
- Medical history.
- Characteristics of the disease (such as inflammation and tumor size).
Minimal Invasive Surgery at Dr. Mehta’s Hospitals
Dr. Mehta’s Hospitals is Chennai’s premier minimally invasive surgery hospital, with the best minimally invasive doctors. Minimally invasive surgeries help patients recover from surgical procedures faster and with less surgical trauma. We offer various types of minimally invasive surgical treatments using advanced technologies and cutting-edge surgical facilities. Visit Dr. Mehta’s Hospitals for your treatment and surgical procedure. Dr. Mehta’s Hospitals offer a variety of day-care surgery options to patients seeking the best surgical experience in Chennai and its surrounding cities.
